GMG Upcoming Events
- >> Click here for upcoming event details! <<
- 6/2 (Tuesday): Breakfast Group, 9:30am
- 6/2 (Tuesday): Collaboration Team Meeting, 2pm, GSC
- HOT! 6/4 (Thursday): Ripped from the Headlines: "Immigration - You Can Help", 2pm, GSC
- FREE! 6/8: MOPOP Tour, 2pm
- 6/15: Bocce ball, 2pm, WPLBC
- 6/18: (Thursday): Walking Group, 10am
- HOT! 6/22: We're Building Tiny Homes!
- [6/24 (Wednesday): Orienteering in Woodland Park, 5pm]
- URGENT! 6/29: "Best Cybersecurity Practices", 2pm, GSC
- 7/6: Pickleball/Cornhole/Games, 2pm, LHCC
Missed an event? Find out what happened here!
Keep Your Teeth, Live Longer and Better
Did you know your mouth is the gateway to your health? And that, as a senior man, keeping your gums in good shape and not losing teeth is strongly correlated with better overall health, lower disease burden, and longer survival?
So, to maintain healthy gums and protect your teeth…
- Have you had your teeth cleaned by a dental hygienist within the past six months?
- Have you had x-rays and a dental exam by a dentist within the past year?
- Do you brush your teeth with an electric toothbrush at least once a day?
- Do you floss every day?
- Do you use an oral irrigator such as a Waterpik?
- Do you use a tongue scraper to remove bacteria from your tongue?
- Eating a diet very low in refined carbohydrates?
- Blood sugar levels well-controlled?
- Avoid mouthwashes containing alcohol?
- Use toothpaste and mouthwashes containing xylitol?
- Don't smoke?
Yeah, no kidding, it can seem to be a hassle to take care of your gums and teeth. Yet it's even more of a hassle to be in poor health and contend with chronic diseases and inflammation.
The Slippery Slope of Poor Oral Health
Gingivitis is a common, mild form of gum disease causing inflammation, redness, and swelling of the gingiva (gum tissue around the base of teeth). It is primarily caused by plaque (a bacterial film) buildup from poor oral hygiene. If left untreated, this early-stage gum infection can progress to serious, irreversible periodontal disease.
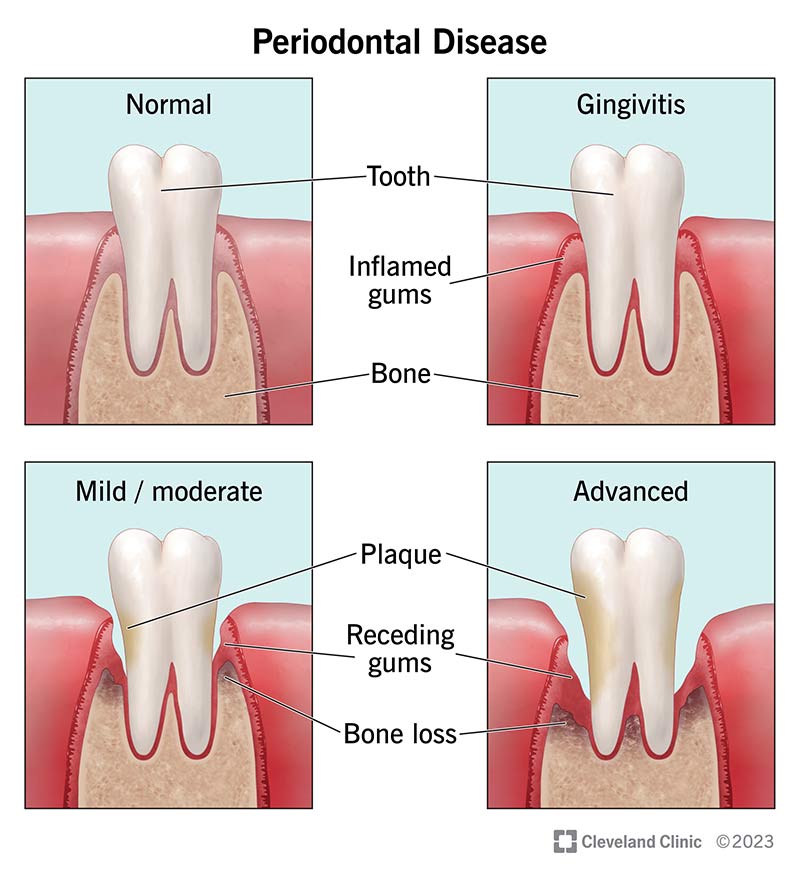
Periodontitis is a serious, chronic bacterial infection of the gums that destroys the soft tissue and bone supporting the teeth, leading to tooth loss if untreated. It stems from untreated gingivitis, where plaque hardens into tartar, creating deep, infected pockets between teeth and gums. Common symptoms include bleeding, swollen gums, bad breath, and receding gums.
We Have a Big Problem
Approximately 60% to 70% of adults aged 65 and older in the United States have some form of periodontal (gum) disease, which includes gingivitis as the initial stage. Periodontal disease is generally more common in men than women, with over 50% of men affected. We hope you are not one of those who are infected.
The problem is that what starts in the mouth doesn't stay in the mouth. It's a visible indicator of your overall health and risk for disease.
Health Researcher Drills Deep into Causes and Solutions for Gum Disease -- and How Your Health Is Affected
To gain a deeper understanding of the vital relationship between healthy gums and avoidance of metabolic diseases, you'll want to view this private seminar with a renowned health researcher.
CAUTION: This seminar is on a password-protected page, intended only for members of the Greenwood men's group.
The password is the first name of the GMG facilitator. His first name begins with a "B".
Click here to gain access to this excellent 30-minute seminar.
Key Links Between Gum Health and Systemic Health
Cardiovascular disease and stroke. Periodontitis is consistently associated with higher risk of heart disease and stroke in older adults; using dental care is linked to lower incidence of both. In older individuals, periodontal disease and tooth loss are associated with higher all‑cause and cardiovascular mortality.
Chronic disease burden and inflammation. Periodontitis contributes to chronic low‑grade systemic inflammation, with bacterial products and inflammatory cytokines entering the circulation and implicated in obesity, diabetes, cardiovascular disease, rheumatoid arthritis, chronic kidney and respiratory diseases, and some cancers. Poor oral hygiene (e.g., infrequent toothbrushing) in middle‑aged and older adults is associated with higher prevalence of chronic diseases, especially cardiovascular disease and diabetes.
Nutrition, frailty, and physical function. Tooth loss and chewing problems in older people impair diet quality and increase risk of malnutrition, frailty, disability, falls, and mortality. “Oral frailty” (multiple deficits such as few teeth, poor chewing, low tongue pressure, swallowing difficulty) may double the risk of physical frailty, sarcopenia, disability, and death.
Mortality and survival in older men. In a Japanese cohort (≥65 years), having no teeth carried one of the highest hazards for death. In the British Regional Heart Study (older men 71–92), tooth loss, dry mouth, and multiple oral problems predicted higher all‑cause, cardiovascular, and respiratory mortality.
Holistic and Mental Health. Poor oral health in older adults is linked to worse quality of life, depression, cognitive impairment, and respiratory infections (e.g., aspiration pneumonia), while better oral status supports physical, mental, and social well‑being.
Why Good Oral Health Matters for Healthy Ageing
Healthy gums (absence of periodontitis) mean less bacterial biofilm, less chronic inflammation, and lower risk of tooth loss. This supports better cardiovascular and metabolic profiles.
Maintaining teeth and oral function supports adequate nutrition, independence, and social interaction, all central to “healthy ageing” as defined by WHO.
Good oral health contributes to better general health status, fewer chronic conditions, improved quality of life, and possibly longer survival in older adults. It also reduces risks of frailty, disability, hospitalization, and mortality in older men.
Happy flossing!
References
1. Meyerhoefer, C., Pepper, J., Manski, R., & Moeller, J. Dental Care Use, Edentulism, and Systemic Health among Older Adults. Journal of Dental Research. 2021; 100. https://doi.org/10.1177/00220345211019018
2. Lipsky, M., Singh, T., Zakeri, G., & Hung, M. Oral Health and Older Adults: A Narrative Review. Dentistry Journal. 2024; 12. https://doi.org/10.3390/dj12020030
3. Nazir, M. Prevalence of periodontal disease, its association with systemic diseases and prevention. International Journal of Health Sciences. 2017; 11.
4. Kotronia, E., Brown, H., Papacosta, A., Lennon, L., Weyant, R., Whincup, P., Wannamethee, S., & Ramsay, S. Oral health and all-cause, cardiovascular disease, and respiratory mortality in older people in the UK and USA. Scientific Reports. 2021; 11. https://doi.org/10.1038/s41598-021-95865-z
5. Kapila, Y. Oral health’s inextricable connection to systemic health: Special populations bring to bear multimodal relationships and factors connecting periodontal disease to systemic diseases and conditions. Periodontology 2000. 2021; 87. https://doi.org/10.1111/prd.12398
6. Kim, M., & Pang, E. Relationship between periodontitis and systemic health conditions: a narrative review. Ewha Medical Journal. 2025; 48. https://doi.org/10.12771/emj.2025.00101
7. Tattar, R., Da Costa, B., & Neves, V. The interrelationship between periodontal disease and systemic health. British Dental Journal. 2025; 239. https://doi.org/10.1038/s41415-025-8642-2
8. Hasan, F., Tandon, A., AlQallaf, H., John, V., Sinha, M., & Gibson, M. Inflammatory Association between Periodontal Disease and Systemic Health. Inflammation. 2025; 48. https://doi.org/10.1007/s10753-025-02317-1
9. Guo, D., Shi, Z., Luo, Y., Ding, R., & He, P. Association between oral health behavior and chronic diseases among middle-aged and older adults in Beijing, China. BMC Oral Health. 2023; 23. https://doi.org/10.1186/s12903-023-02764-y
10. Hwang, S., & Yu, J. Relationship between Chronic Disease, Oral Health Behavior of Elderly and Periodontal Disease. Journal of the Korea Academia-Industrial cooperation Society. 2024 https://doi.org/10.5762/kais.2024.25.5.116
11. Liu, F., Song, S., Ye, X., Huang, S., He, J., Wang, G., & Hu, X. Oral health-related multiple outcomes of holistic health in elderly individuals: An umbrella review of systematic reviews and meta-analyses. Frontiers in Public Health. 2022; 10. https://doi.org/10.3389/fpubh.2022.1021104
12. Nakazawa, N., Kusama, T., Cooray, U., Yamamoto, T., Kiuchi, S., Abbas, H., Yamamoto, T., Kondo, K., Osaka, K., & Aida, J. Large contribution of oral status for death among modifiable risk factors in older adults: the JAGES prospective cohort study.. The journals of gerontology. Series A, Biological sciences and medical sciences. 2022 https://doi.org/10.1093/gerona/glac052
13. Dibello, V., Lobbezoo, F., Lozupone, M., Sardone, R., Ballini, A., Berardino, G., Mollica, A., Coelho-Júnior, H., De Pergola, G., Stallone, R., Dibello, A., Daniele, A., Petruzzi, M., Santarcangelo, F., Solfrizzi, V., Manfredini, D., & Panza, F. Oral frailty indicators to target major adverse health-related outcomes in older age: a systematic review. GeroScience. 2022; 45. https://doi.org/10.1007/s11357-022-00663-8
14. Natarajan, P., Madanian, S., & Marshall, S. Investigating the link between oral health conditions and systemic diseases: A cross-sectional analysis. Scientific Reports. 2025; 15. https://doi.org/10.1038/s41598-025-92523-6
15. Tanaka, T., Takahashi, K., Hirano, H., Kikutani, T., Watanabe, Y., Ohara, Y., Furuya, H., Tetsuo, T., Akishita, M., & Iijima, K. Oral Frailty as a Risk Factor for Physical Frailty and Mortality in Community-Dwelling Elderly. The Journals of Gerontology: Series A. 2018; 73. https://doi.org/10.1093/gerona/glx225
16. Liu, W., Chuang, Y., Chien, C., & Tung, T. Oral health diseases among the older people: a general health perspective. Journal of Men’s Health. 2020 https://doi.org/10.31083/jomh.v17i1.316
17. Sadighi, T., Dzioba, C., & Churaman, B. Poor Oral Health in the Elderly and Its Effect on Chronic Disease. The Journal for Nurse Practitioners. 2023 https://doi.org/10.1016/j.nurpra.2023.104782
18. Chan, A., Tsang, Y., Chu, S., & Chu, C. Comprehensive Strategies for Preventive Periodontal Care in Older Adults. Geriatrics. 2025; 10. https://doi.org/10.3390/geriatrics10030072
The mission of of seattleseniormen.com and greenwoodmensgroup.com is to provide a supportive environment where men from diverse backgrounds can foster camaraderie, develop friendships, share wisdom, enrich one another's lives -- and contribute to all Seattle communities, including Greenwood, Ballard, Crown Hill, Fremont, Green Lake, Licton Springs, Loyal Heights, Magnolia, Phinney Ridge, Ravenna, Sunset Hill, Wallingford, Wedgwood, Whittier Heights. Bitter Lake, Broadview, Haller Lake, Queen Anne, and beyond.
Recent Articles
-
Greenwood Men's Group - Upcoming Events and Activities in Seattle Area
Jun 01, 26 09:39 PM
List of upcoming events for the Greenwood Men's Group in Seattle -
Greenwood Men's Group in Seattle - Archive of Past Events
Jun 01, 26 08:04 PM
Here's what happened in past events of the Greenwood Men's Group in Seattle -
Curmudgeon's Cave - Greenwood Men's Group Member Speaks Out
May 28, 26 12:05 AM
Observations and Opinions from a Greenwood Men's Group member